As most anyone of the millennial generation surely knows, there has been a huge emphasis on surgical simulation in the modern era of ophthalmic training. Rightfully so, instead of doing one’s first case on a living, breathing vulnerable patient, one can now do hundreds if not thousands of virtual cases beforehand. Not only are our patients better protected, but the saintly attendings who staff cases in July are as well. Even though this month’s Tech Culture column will appropriately focus on the high-tech EYESi Virtual Reality Simulator (VRMagic), it is certainly not the only available option for realistic surgical simulation. The classic low-tech pig or cow eye wet lab still has many virtues and should continue to be an integral part of any modern surgical curriculum. The use of a real phaco machine will always trump a virtual one, and real eyes will always be better for tissue handling, wound creation, suturing, and virtually all corneal procedures.
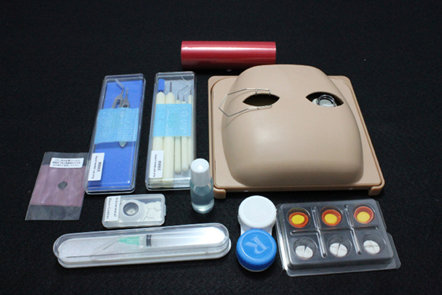
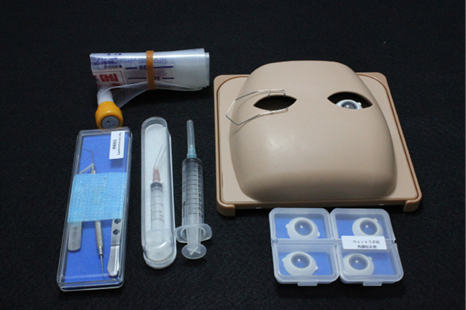
The Kitaro phac eye (Frontier Vision) (get it?) is another great simulation option falling in the mid-tech category between the animal eye and the EYESi simulator. It is a highly sophisticated 3D eye model, which, in my opinion, more realistically simulates most of the critical steps in cataract surgery than animal eyes (plus you get to avoid the stench of rotting eyes, which inevitably invades every refrigerator in every wet lab everywhere). The Kitaro system, in my opinion, is as good as, if not better than, the EYESi system at capsulorhexis and phacoemulsification with the distinct advantage of using a real phaco machine at a substantially reduced entrance fee. The dry lab portion of Kitaro allows residents to practice unlimited capsulorhexes in the comfort of their own homes—an impossible feat with the EYESi. The EYESi has many advantages of its own, and since this is a tech column, it will be featured below. My colleague, Ana Alzaga Fernandez, who I never knew was a Trekkie, has plenty of experience with the simulator and has graciously contributed this month’s article.
—Christopher E. Starr, MD
In Star Trek, the Emergency Medical Hologram or EMH is a holographic program intended to teach medical personnel aboard a Starfleet vessel how to proceed in case of an emergency. Yes, I am a newly self-proclaimed Trekkie. I’ve always been a late bloomer, and I recently discovered the captivating world of Star Trek. I love it because, just as with many other things, including virtual reality (VR) for training purposes, the writers of Star Trek were thinking way ahead of their time.
From “see one, do one, teach one” to “see one, simulate one, do one, teach one” to boldly go where no man has gone before! The Halstedian apprentice model has served as the basis for surgical instruction for more than 100 years in all areas of medicine, including our very own field of ophthalmology.
So, what have we learned when teaching/learning cataract surgery under this model? Well, evidence surely supports that surgical competency as measured by complication rates and phacoemulsification efficiency indeed improves after the first 80 cases.1 About that learning curve, we can only say, buckle up. Perhaps you now know the real meaning of “out ... of ... the ... chair.” Early on, it is quite helpful to carefully select the appropriate patients for optimal surgical results in cases done by trainees.2,3
We know that a standardized cataract surgical training course, with wet lab sessions and subjective and objective assessment tools, serves as a solid learning tool.4,5 A uniform surgical curriculum, such as the OWL program from the University of Iowa, that emphasizes the importance of faculty-assisted wet labs when the residents are first introduced to the OR is crucial.5,6 Highly not illogical, right?
OK, but what if pigs’ eyes are not your thing? Well, as Spock would say, I like to believe that there are always possibilities, and I couldn’t agree more with him. The Kitaro WetLab system is a great alternative to porcine wet labs, which offers the ability to practice surgical techniques using synthetic but realistic materials most of which are reusable. There are wet and dry kits and also complex case kits to practice cases with small pupils, weak zonules, transscleral fixation of IOLs, and even extra caps.
But how about an effective computerized VR system that could also serve as a great tool for learning cataract surgery? Fascinating, tell me more.
Along comes the EYESi Ophthalmic Surgical Simulator. Currently, it is the only VR system available for cataract surgery training. It includes a quad camera optical tracking, patient interface (head), hand-activated forceps, multiple modules (including capsulorhexis, phaco chop, hydro dissection, I/A), scoring rubrics for skill assessment, and a surgical training curriculum.
I know what you are thinking, “This isn’t reality. This is fantasy.” Or rather ... an alternate reality.
What else can you tell me about the EYESi, Scotty? Beam us up!
Construct validity has been proven for forceps, anti-tremor, capsulorhexis, phaco, cracking and chopping, and avigation modules.7,8,9 Many studies have looked at its impact on residents’ cataract surgical performance:
• Belyea et al, shorter phacoemulsification times and lower power, fewer intraoperative complications.10
• Feldman et al, trend toward improved surgical skills.11
• Feudner et al, superior wet lab capsulorhexis performance.12
Permission to speak freely, sir? Here is my take: I like this ship! You know, it’s exciting! I had access to it during my 3 years of residency training, and I used it quite frequently, even towards the end of my third year. In a small study my peers and I conducted, we found that it shortens the learning curve in the first 50 cases. Our attendings, who have taught residents before and after incorporating the EYESi into our surgical curriculum, agree that it has decreased the need for their intervention and it has improved capsulorhexis performance in the OR.13
Finally, the International Forum of Ophthalmic Simulation or IFOS, a global collaborative program, determined that a structured simulation program at an early stage provides a significant degree of skill to novice ophthalmic surgeons, although involvement of a senior trainer offering guided supervision is critical.14
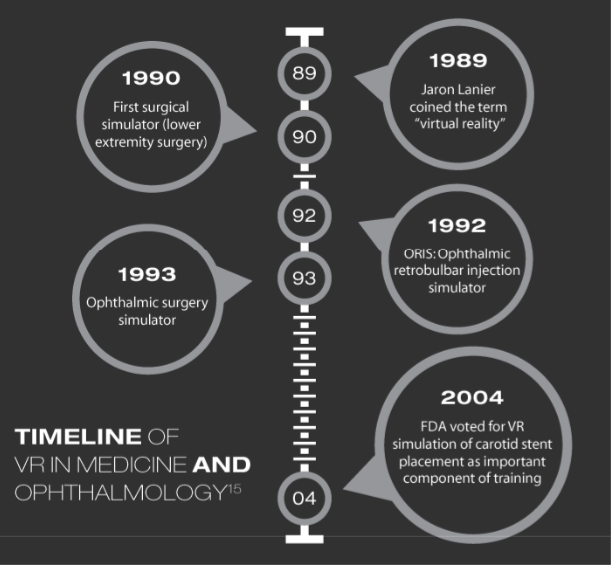
In conclusion, VR training in ophthalmology is most likely here to stay and can serve as a very valuable tool for trainees. Space, or rather excellence in cataract surgery training, is the final frontier. Live long and prosper.




