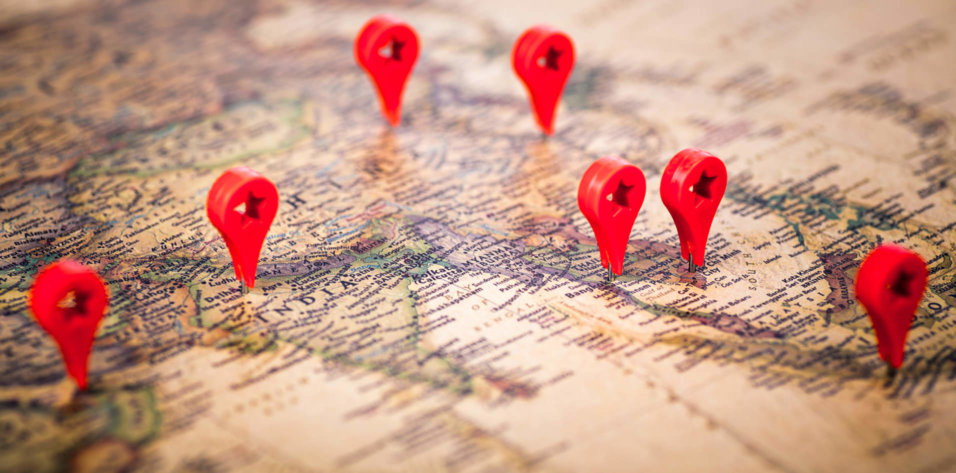
In the United States, surgeons schedule corneal transplant procedures with the same freedom as cataract surgery, knowing donor tissue is as readily available as any IOL. Of course, surgeons are aware that donor tissue is not manufactured; it arrives at the OR at the end of a meticulous process that begins with a generous final act. Here’s how that process works.
DONATION AND RECOVERY
Donor identification can happen in several ways, depending on the cause of death. Generally, when a patient is pronounced dead or brain death has occurred, that patient is considered a potential organ and tissue donor. Each state has its own process by which the hospital notifies the appropriate agency and reviews whether the patient is a registered donor or obtains family consent for donation. In all cases, the family is asked about the patient’s medical and social history to help determine transplant eligibility.
While this is happening, physicians evaluate the potential for major organ donation—a high priority—as well as for tissue donation. Many factors can rule out a potential donor, including a history of certain cancers, infectious diseases, or serology testing that shows the presence of HIV or hepatitis B or C. A donor coordinator manages the recovery process while agencies like the Indiana Lions Eye Bank arrive to begin our recovery, storage, and distribution protocols.
When the donor’s heart is stopped, the clock starts. Organ recovery occurs first, while the respective agencies coordinate waiting recipients. Tissue recovery follows next.
Corneal tissue can be recovered within 8 to 10 hours. Corneal excision takes a few minutes for each eye. Each cornea is preserved in a separate container in media that supports storage for up to 14 days.
EVALUATION AND PREPARATION
When the donated tissue arrives at the eye bank, we evaluate it for transplantation. A slit-lamp examination informs us of any previous surgery, physical defect such as post-infection scarring, or pathology that precludes use. The specular microscope reveals the number of endothelial cells in the tissue as well as which layers are suitable for various procedures.
The eye bank deems a cornea suitable for transplantation if the stroma has a smooth surface with no epithelial damage, no scars or visual defects, and the requisite endothelial cell density. Of all the donor tissue available, our screening process approves 60% to 70% for some form of transplantation. Much of the remaining 30% to 40% is suitable for research, education, and the practice of new surgical procedures.
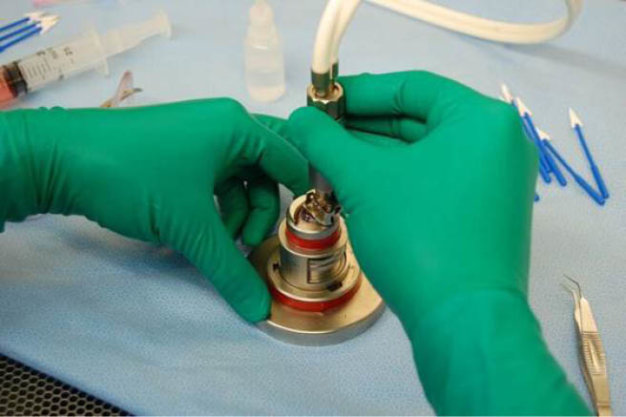
Figure 1 | Using a microkeratome, the technician removes the outer three-quarters of the cornea to prepare it for Descemet stripping automated endothelial keratoplasty (DSAEK) surgery. The remaining tissue graft is approximately 100-µm thick. Tissues are cut to within ±30 µm of the requested thickness.
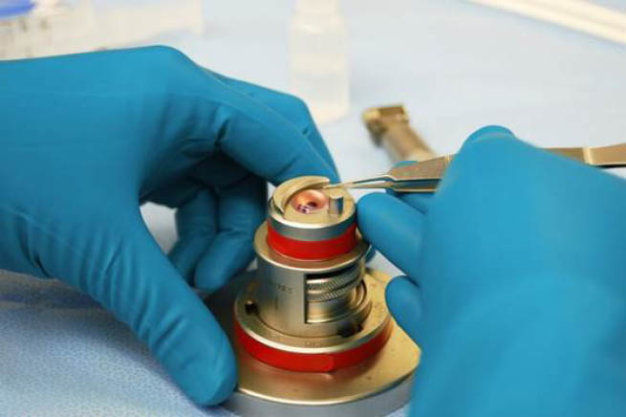
Figure 2 | Tissue has been pre-cut for DSAEK. The technician is replacing the cap, measuring 10 mm in diameter and between 400 µm and 500 µm in thickness, at the end of the cut.
It is our job as a nonprofit eye bank to fulfill requests from surgeons, including providing the prepared tissue needed for any corneal procedure (Figures 1 and 2). For transplant procedures, most surgeons prefer tissue that is young but mature enough to be easily manipulated. They want an endothelial cell density between 2,000 and 3,500 cells/mm2. A high end cell density is desirable for Descemet membrane endothelial keratoplasty (DMEK) because only the single-layer, 15-µm-to-20-µm-thick Descemet membrane will be transplanted.
REGIONAL AND INTERNATIONAL DISTRIBUTION
Timing is key to distributing donated tissue. There is a 1- or 2-day delay between recovery and distribution. If we have a recovery one day, we evaluate the tissue the next morning and await the serology results, which typically take a day. Surgeons post their scheduled surgeries online and then contact us a few days in advance to ask what tissue we have available.
We distribute tissue across a large geographic area. Eye banks were originally formed to meet a community need—in the case of my organization, that of the state of Indiana—but it makes sense to work beyond our boundaries. As part of the nonprofit Vision Share consortium of eye banks, we are able to efficiently distribute excess corneas as well as to find tissue to meet our local needs when we have a deficit. Because eye banks in the United States actually have more tissue than patients require, Vision Share has the distribution network to export tissue to where it is needed around the world (Figure 3).
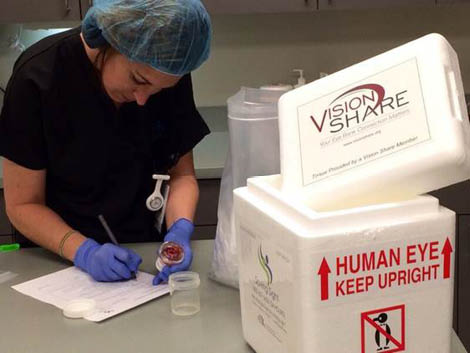
Figure 3 | Vision Share distributes prepared corneal tissue to surgeons in the United States and abroad.
After distribution, our organization verifies that the tissue was used and documents the recipient. As a final step, we follow up to make sure that the outcome was positive as part of our quality improvement measures for regulatory compliance.
EDUCATION THROUGH EYE BANKS
In addition to their primary functions of recovering, preparing, and distributing donated corneas, eye banks also advance transplantation by helping surgeons adopt new procedures. We encourage doctors to contact us for practice corneas and practice grafts such as those used for DMEK and other procedures. Surgeons also can use our facility’s wet lab, where our microscope is available for practice sessions with donated tissue. You will find that any nonprofit eye bank you work with will welcome your visit for a behind-the-scenes look at our work.