Putting yourself first—it’s a simple solution to a simple problem, right? Yoga, meditation, and mindfulness form the ultimate wellness trifecta, and, if we focus on these practices, we’ll be good to go for the rest of our lives. This is what we’re often told. But, in actuality, the concept of putting yourself first is a complex solution to a complex problem. As a certified yoga instructor with a personal meditation practice, I can tell you that these practices can be key components of self-care. But one size does not fit all, and we each have to find what works for us as individuals.
WHY PRIORITIZE YOURSELF
An epitaph of an Athenian doctor from 2 AD reads, “These are the duties of a physician. First, to heal his mind and to give help to himself before giving it to anyone else.” For thousands of years, we have known the importance of self-care, yet for some reason self-care tends to fall down to the lowest spot on physicians’ lists of priorities.
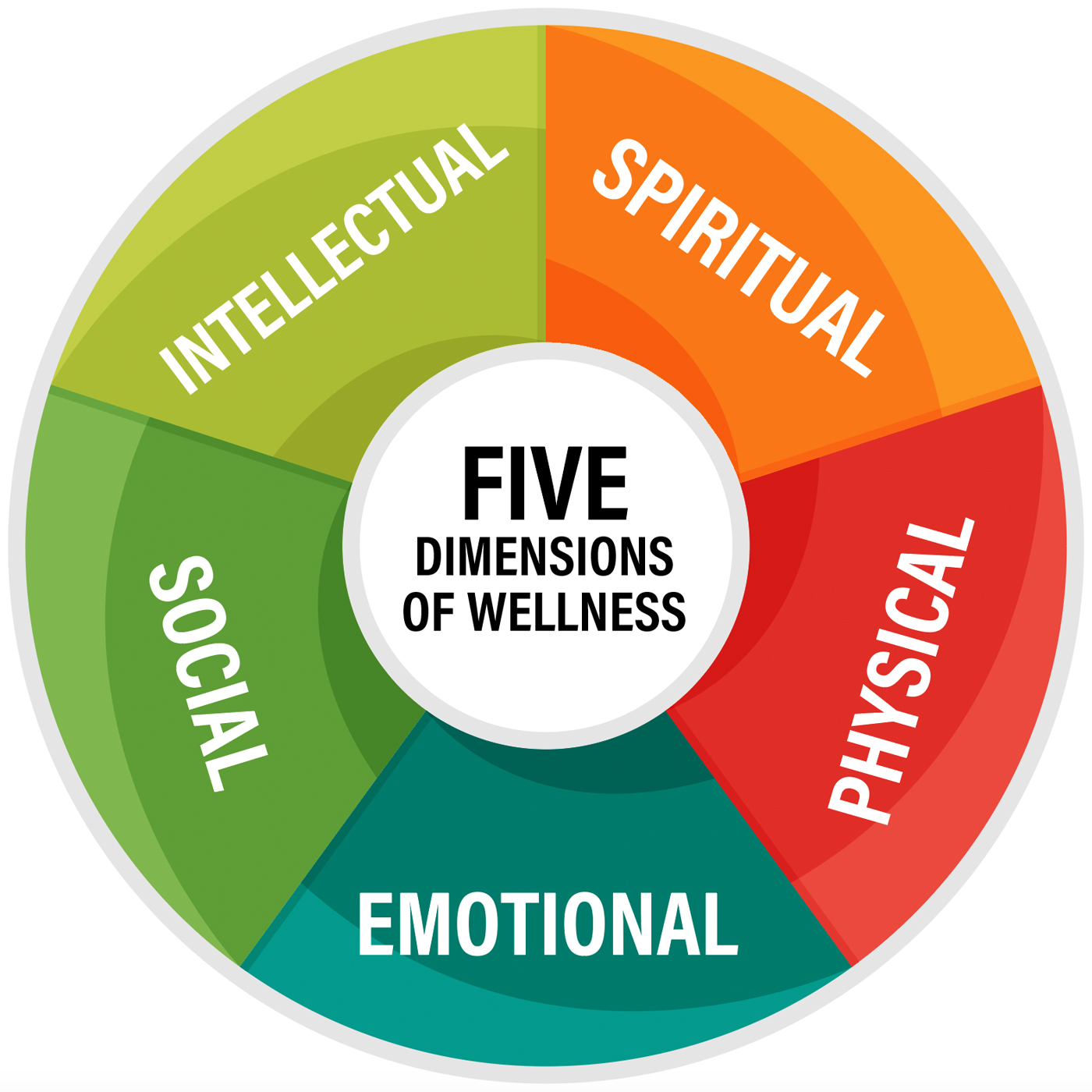
Why is self-care so important? The World Health Organization defines optimal health as a state of optimal wellbeing, not merely the absence of disease and infirmity. Wellness is often thought to have five dimensions: emotional, physical, spiritual, intellectual, and social. Emotional wellness relates to the process of accepting our worth, expressing our feelings, and talking to ourselves in healthy ways. Physical wellness involves nutrition, fitness, sleep, and stress management. Spiritual wellness reflects our ability to discover meaning and purpose in life. Intellectual wellness—where physicians excel—is the ability to use our minds to set and achieve career, educational, and financial goals. Social wellness involves the ability to cultivate stable relationships and find security in a social network.
Essentially, the why behind the need for self-care comes down to this: burnout. Burnout is not new, but it is real and increasing in prevalence. Many people think burnout is simply an inability to handle day-to-day stressors. But, in reality, burnout is a syndrome of emotional exhaustion, depersonalization, and a reduced sense of accomplishment, and it can be devastating. Although burnout affects individuals in all fields of work, physicians have shown a faster increase in rates of burnout in the past decade compared with other fields. Interestingly, women are at greater risk. In a field where women now comprise 50% of medical students, this trend needs to be evaluated and better understood.
MYTHS WE TELL OURSELVES
As physicians, many of us tell ourselves that self-care is unimportant. We may perceive prioritizing our wellness as a selfish act, when we should be more concerned with our patients’ well-being. We may also tell ourselves that we have no time for self-care. Yet, interestingly, physicians are less effective and less efficient at taking care of patients when they are burned out.
Further, we may tell ourselves that it is not necessary to worry about our wellness. We put on our superhuman capes and say, “We’ve got this.” But that is not sustainable. When a physician who burns out becomes less effective and less efficient at caring for his or her patients, that burden is transferred to other physicians in his or her practice or program. It becomes a vicious cycle in which everyone will eventually burn out.
The American Medical Association looked at how burnout affects different medical specialties. Those of us in ophthalmology may assume we took the road to happiness with our chosen specialty and that urologists and neurologists are the specialists burning out. But ophthalmology still has a 34% rate of burnout. One in three of your colleagues is burned out right now—that is not acceptable.
Why are physicians more prone to burning out? First, we possess a certain set of characteristics that got us through our rigorous training—ie, compulsiveness, self-denial, delayed gratification, and sleep deprivation. Our training inherently involved a denial of personal vulnerability. One of my gurus in whole living, Brené Brown, talks about how important it is to be vulnerable. Yet, we are the least willing to allow ourselves that opportunity.
Physicians are also more prone to burnout because we work in a medical culture that emphasizes perfectionism. Our patients expect us to know why they have a problem, when we can fix it, and why it wasn’t fixed yesterday. Further, our personal tendencies outside of being a physician, including self-criticism and perfectionism, make us more susceptible to burnout.
Those of us without children may think that we shouldn’t be burned out because we have all the time in the world to focus on ourselves. However, studies have shown that not having a spouse or child is actually a higher risk factor for burnout because having that close support system forces individuals to seek out a better work-life balance.
Overall, greater empathy leads to a higher risk of burnout. Medicine calls for providers who are empathetic. Our patients want to be cared for by a provider with the ability to empathize, yet that very empathy increases our risk of burnout.
STEPS TO SELF-CARE
Stay curious. Be aware of how stress presents in you and think about what might help you to combat it. For me, yoga and meditation work. Others may benefit from hiking 3 days a week or speaking to a friend once a week. Whatever the practice, you must give yourself that time and commit to it. Understand that how you deal with stress today may be different in 10 years. Don’t allow yourself to get transfixed on one way of coping.
Keep calm and delegate. Fortunately, practicing physicians are often in a financial situation that enables them to delegate certain responsibilities. For example, I despise cleaning and folding laundry, so I outsource these tasks. If you don’t enjoy cooking, subscribe to a meal service. Don’t allow yourself to feel like you have to do it all. Ask for help.
Have a group. Find a group of individuals who will advocate for you. Be willing to be vulnerable with your colleagues and say, “Listen, I’m struggling right now. How have you’ve dealt with that?” We have all struggled, and we’ve all tried to come up with ways to address it. Sometimes just the ability to express your feelings will help.
Schedule your self-care. It is imperative that you schedule time for self-care. It has to be a part of your regular routine, or it won’t happen.
Forgive yourself. If you’ve said that your self-care will be 20 minutes of meditation every day and suddenly 4 days have passed and you haven’t meditated, forgive yourself. Beating yourself up won’t help anyone. Rather, break your self-care into digestible practices—take 1 minute when you get to work to sit in your car and breathe. Then when you get home, take that same minute to breathe. Give yourself the opportunity to adapt and stay flexible. It will make all the difference in your self-care success.



