Toric IOLs are a shining example of advanced technology for cataract surgery. They allow surgeons to achieve excellent postoperative refractive results for patients with astigmatism. As with any technology, however, there are times when the clinical results fall short of expectations. Fortunately, multiple resources are available to help surgeons evaluate patients with residual postoperative refractive error after toric IOL placement.
THE STANDBY
Clearly, many surgeons are familiar with the Berdahl-Hardten Toric Results Analyzer, given that www.astigmatismfix.com has been accessed more than 20,000 times in the past 2 years. A powerful and intuitive tool, this calculator has enabled surgeons to manage residual astigmatic refractive errors after the placement of a toric IOL. The ophthalmologist enters some basic biometric data and a postoperative refraction, and then, the calculator determines how much rotation of the lens is needed to achieve the lowest amount of residual astigmatism. Although extremely helpful, this tool does not indicate whether changing the spherical and/or toric power of the IOL would also improve the postoperative refractive outcome.
A MORE ROBUST OPTION
An even more robust tool is now available for assessing postoperative refractive errors. The Barrett Rx Formula uses both the Barrett Universal II formula and the Barrett Toric Calculator to perform its analysis. Not only does the Barrett Rx Formula provide anterior segment surgeons with information that identifies how much to rotate the toric IOL in a patient with residual ametropia, but it also determines whether exchanging and/or rotating the IOL to adjust spherical and toric powers will improve the postoperative refractive result. Additionally, surgeons can use the Barrett Rx Formula to calculate the appropriate strength of a piggyback IOL for a patient who has experienced a refractive surprise.
WHERE TO FIND IT
Surgeons can access the Barrett Rx Formula through a link in the tools area of the ASCRS website (https://www.ascrs.org), which will take them to the Asia-Pacific Association of Cataract and Refractive Surgeons’ website.
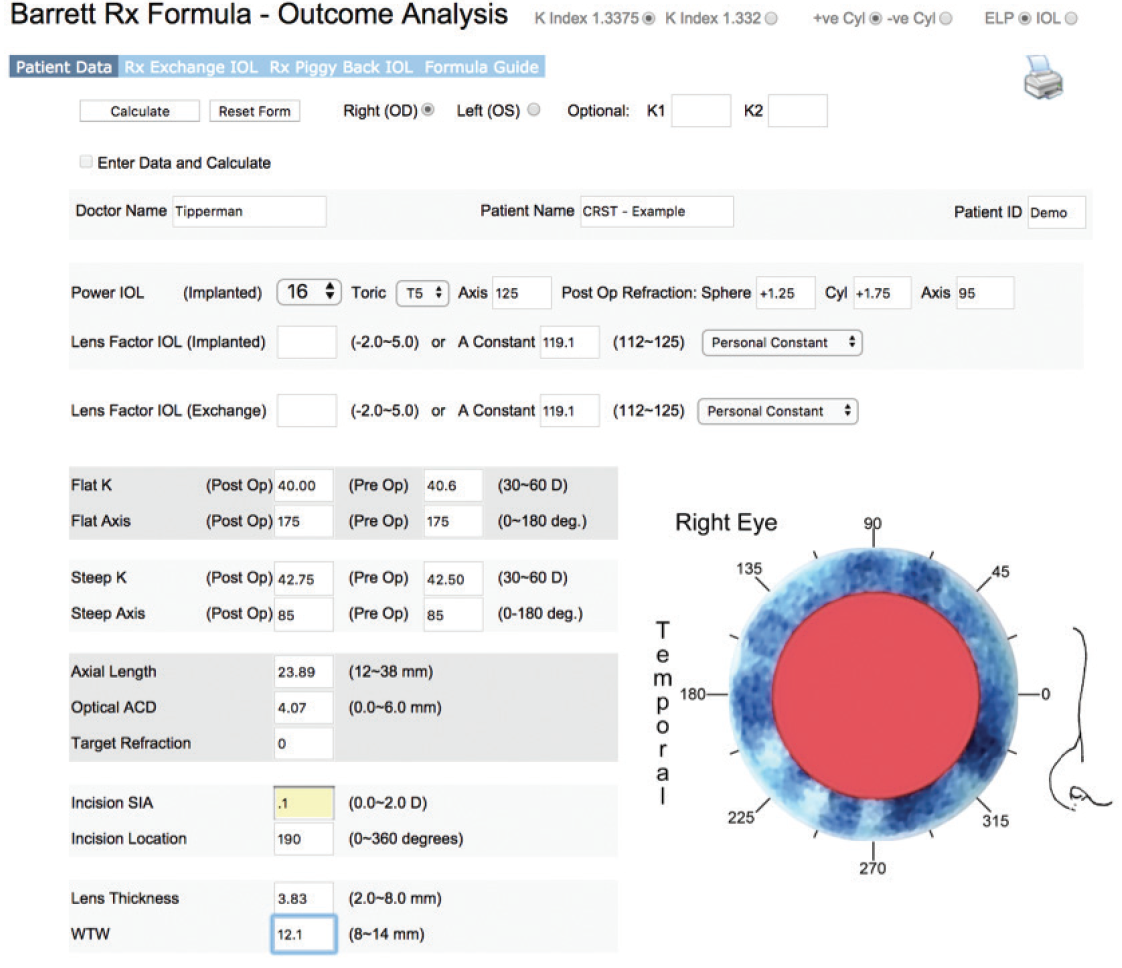
Figure 1 | The author enters data into the Barrett Rx Formula for a hypothetical case example.
HOW IT WORKS
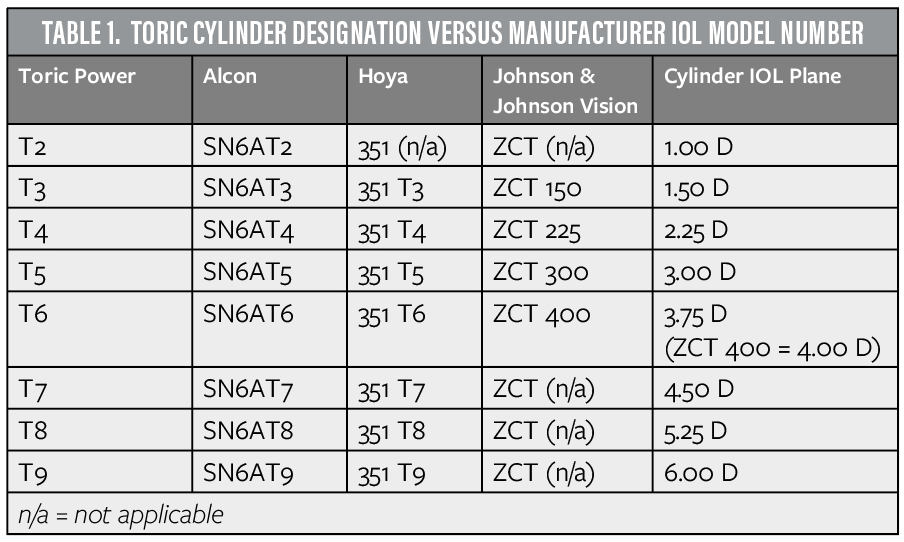
The main data entry screen, shown in Figure 1, is populated with data to demonstrate a hypothetical case discussed later in this article. After some general demographic data, the webpage has boxes in which to enter information regarding the implanted toric IOL. The calculator is agnostic with regard to IOL manufacturer. If surgeons are not certain which toric power (T power) to designate, however, they can view the appropriate powers by clicking on the formula guide box, which provides additional information on using the calculator, including appropriate T powers for each IOL company (Table 1). If the surgeon will be exchanging the IOL for a different lens, he or she may indicate the A-constant of the new IOL. Similarly, if the surgeon is planning to change from capsular bag to sulcus fixation, he or she may note the appropriate A-constant.
In the hypothetical case displayed in Figure 1, the surgeon implanted a 16.00 D »AcrySof IQ Toric IOL (model SN6AT5 IOL; Alcon) at an axis of 125º. The patient’s current refraction is +1.25 +1.25 X 095º. Below these data, the surgeon enters the A-constant for both the implanted IOL and the IOL to be used if an exchange is performed, followed by the patient’s pre- and postoperative keratometry readings and associated biometric measurements. After entering all of these data, the surgeon clicks the Calculate button, and the webpage appears (Figure 2), with the steep and flat meridians indicated on the picture of the eye in the lower right–hand corner. This gives the surgeon one final step to confirm all the data.
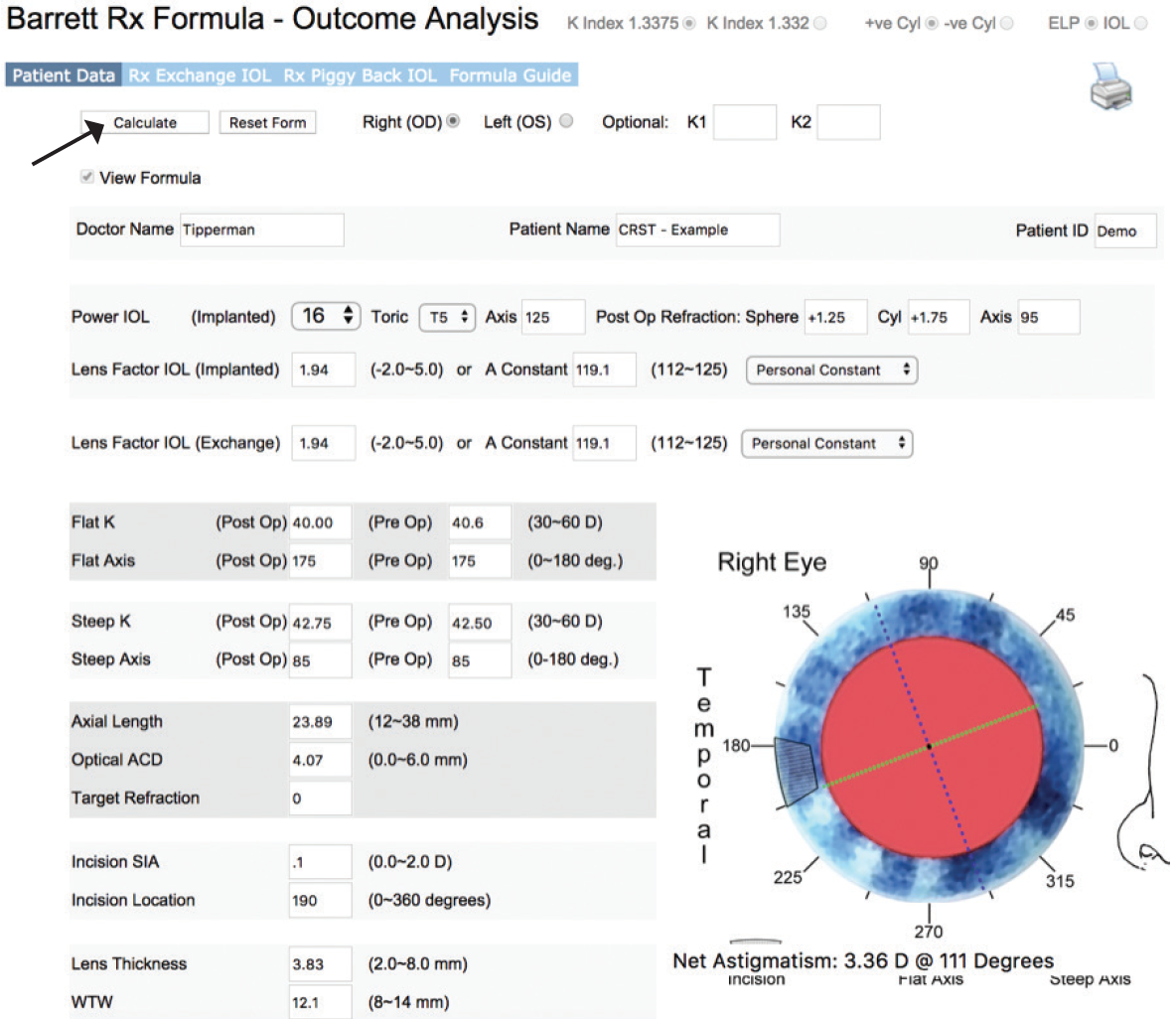
Figure 2 | After data input is complete, the surgeon clicks the Calculate button and confirms the data.
After verification is complete, the surgeon clicks the blue Rx Exchange IOL tab at the top left of the page. The results displayed demonstrate how powerful the Barrett Rx formula is for analyzing IOL power surprises (Figure 3). In this hypothetical case, the first set of information demonstrates that exchanging the 16.00 D SN6AT5 IOL for an 18.50 D SN6AT7 IOL will yield a final spherical equivalent refraction of 0.02 D. Separately displayed data show the refractive results of changing both the spherical and toric powers.
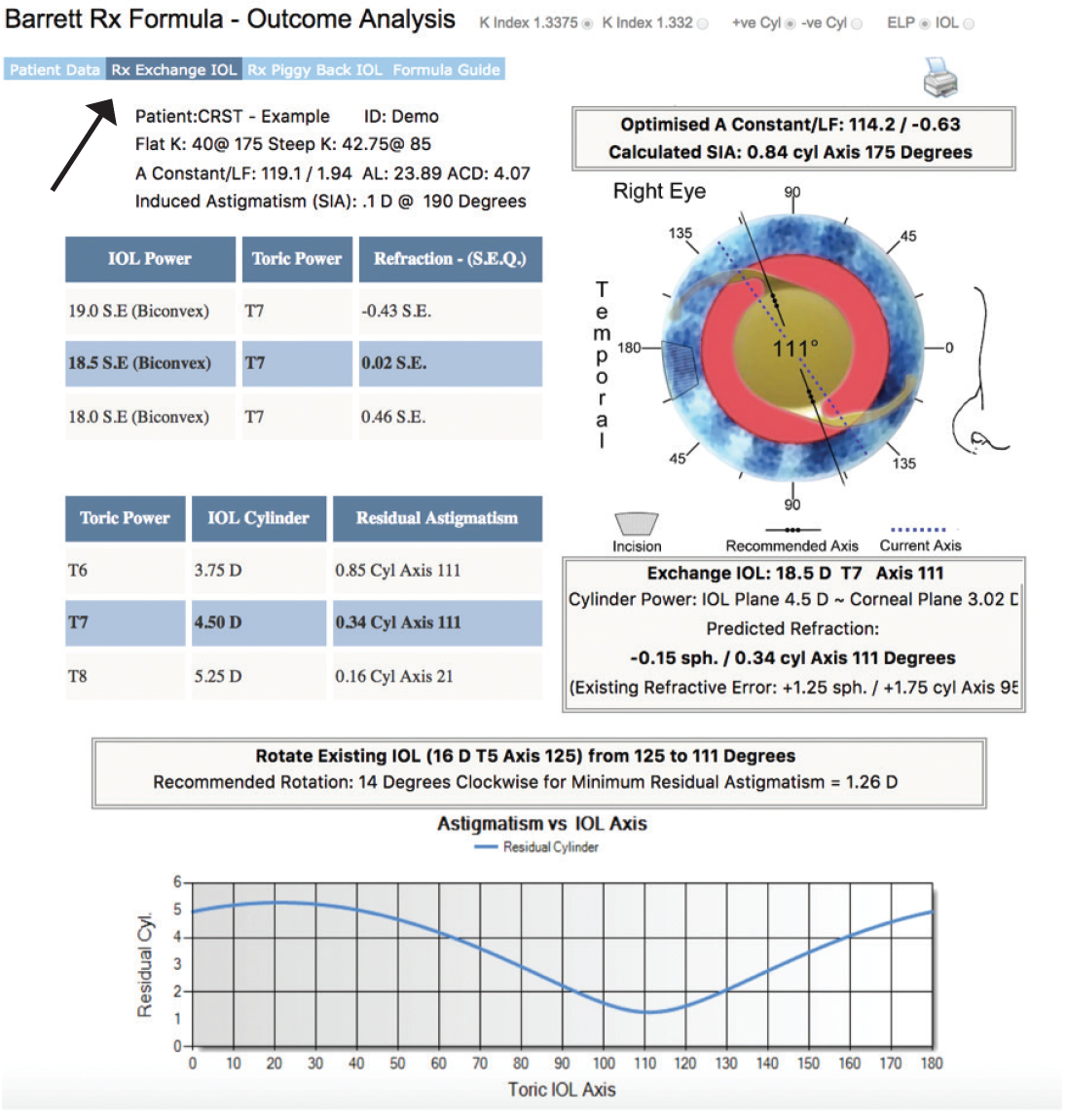
Figure 3 | After the surgeon clicks the blue Rx Exchange IOL tab, the Barrett Rx Formula not only shows how much to rotate the current IOL, but it also demonstrates how exchanging the lens for an IOL with different spherical and toric powers would affect the refractive result.
In the schematic eye portion of the webpage, the surgeon can review a summary of the current IOL and refraction as well as the recommended IOL and theoretical refraction. Finally, a graph similar to that provided by the Berdahl-Hardten calculator shows the refractive results that will be obtained by just rotating the currently implanted IOL without exchanging it for a differently powered IOL.
CONCLUSION
Toric IOLs are an excellent option for achieving desirable refractive results in patients with astigmatism who require cataract surgery. As with any technology, however, the occasional outcome will not be optimal. The Barrett Rx Formula represents a major advance in the management of these outliers.



