Case No. 1
These videos demonstrate a case of same-day sequential bilateral cataract surgery in an intellectually challenged patient with brunescent cataracts, who required general anesthesia. Hyaloid-sparing posterior continuous curvilinear capsulorhexis and posterior optic capture were performed in both eyes, providing a clear visual axis for the patient's lifetime.
Case No. 2
An 11-year-old boy presented with near-total hyphema after a BB gun bullet hit the closed lid of his right eye. He had hand motion vision and an IOP of 30 mm Hg OD. No reverse afferent pupillary defect was observed. The patient was managed conservatively with steroids and topical dorzolamide-timolol ophthalmic suspension 2%/0.5% (Cosopt, Akorn) and brinzolamide (Azopt, Alcon). The eye quieted, the hyphema was absorbed, and IOP was controlled. Two months later, the patient underwent cataract surgery.
PEARLS FOR MANAGING TRAUAMTIC CATARACTS
- Avoid irrigation and turbulence
- Identify structures
- Maintain the anterior chamber
- Compartmentalize
- Expose the trabecular meshwork
- Avoid cautery
- Prepare the patient for more than one surgery
After the cataract procedure, the eye was quiet, visual acuity was 20/60, and the IOL was centered. Posterior capsular opacification was observed, so the patient was tapered off the glaucoma medications and, 10 weeks later, underwent an Nd:YAG laser capsulotomy. Six weeks later, the patient returned with iritis after sustaining a dodgeball injury. Retraction of the iris revealing entanglement of the haptic with presumed IOL instability prompted a second surgery. A one-port pars plana anterior vitrectomy and posterior capsulotomy enlargement with intended optic capture into the Berger space were planned. Intraoperative inspection showed a stable lens. Amputation of the haptic, removal of a knuckle of herniated vitreous, and pupilloplasty were performed, as shown in the video.
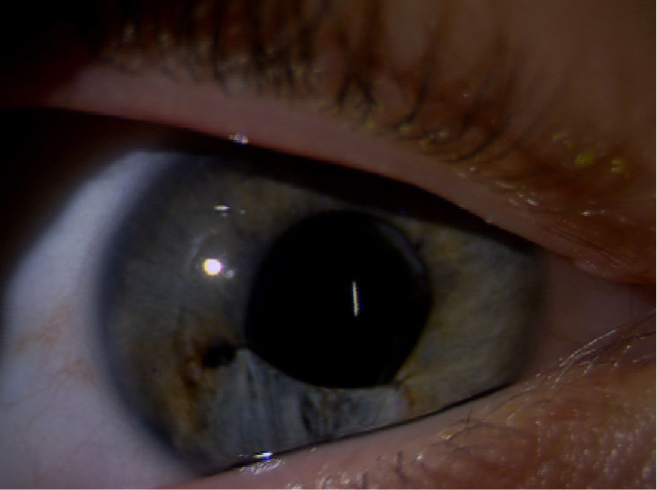
Figure | Anterior segment reconstruction following two ocular injuries.
At 4 months postoperatively, the patient was off all drops, IOP in the treated eye was symmetric with that of the untreated eye, and no retinal pathology was present. Vision corrected to 20/20 from 20/25, and the patient was comfortable with excellent cosmesis (Figure). Plus, he now wants to become an eye surgeon!



