Evidence-based medicine (EBM) refers to the process of obtaining and applying the best scientific data to daily medical practice. This approach advocates that medical practice not be based solely on the beliefs of practitioners or experts or on nonsystematic clinical observations and personal experiences.
Instead, the EBM paradigm is supported by three pillars: (1) individual clinical expertise, (2) the best available research and its critical analysis; and (3) patient values, circumstances, and preferences. The logic is that, through their integration, physicians can optimize their decision-making processes for improved patient care.
Individual clinical expertise is shaped by both skill and judgment, which physicians develop through their daily practice. It involves the capacity to efficiently identify a patient’s clinical condition, issue a diagnosis, and weigh the risks and benefits of available interventions. Such expertise is also strongly linked to the physician’s ability to locate the best published evidence on a patient’s condition and to determine the appropriate treatment that best takes his or her values and desires into consideration.
The practice of EBM involves at least five steps, as detailed below.
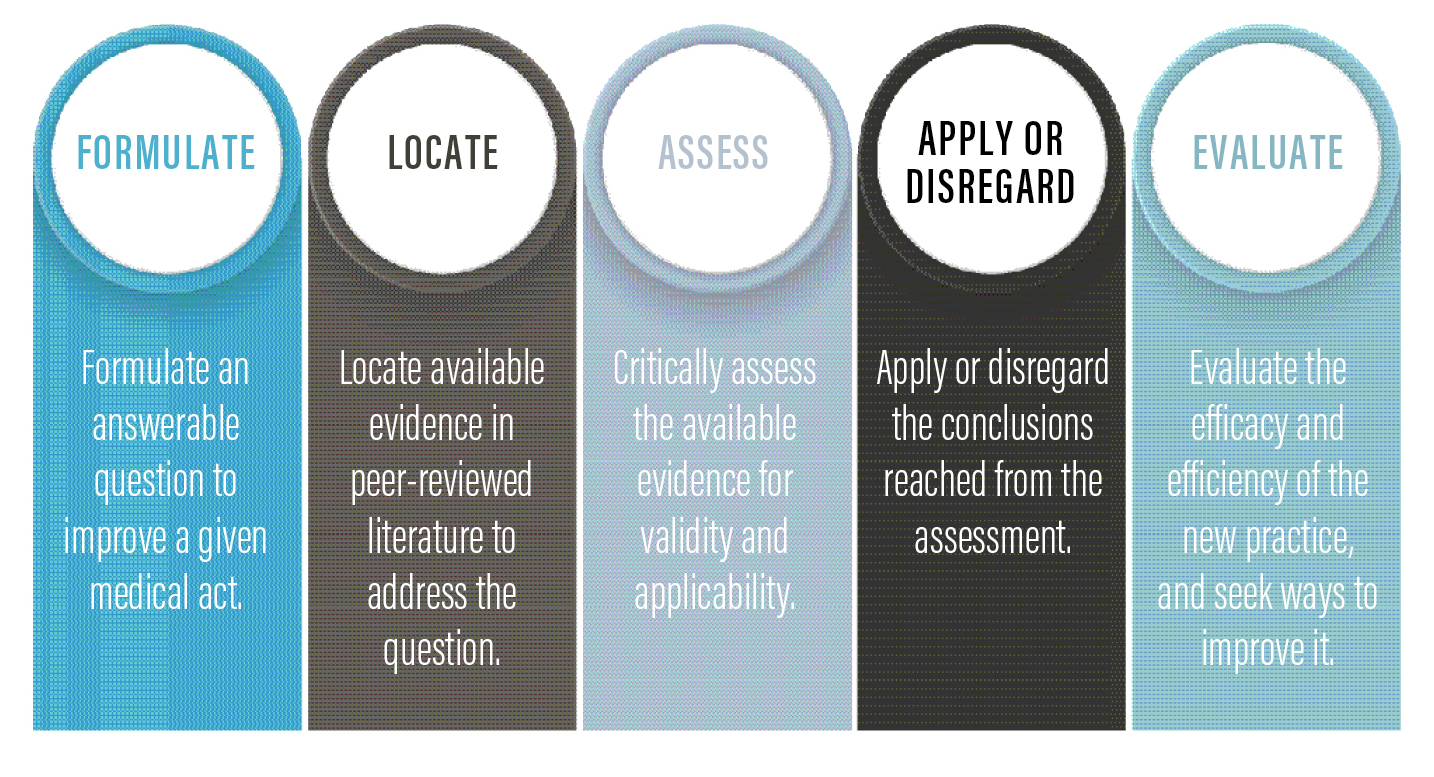
ADVANTAGES OF EBM
The practice of EBM offers several advantages to the practitioner. It enables critical assessment of both established and newly discovered information, and it can reduce the time between acquisition and application of knowledge. It encourages reflective medicosurgical practice and helps minimize unnecessary treatment or overtreatment; thus, EBM may also yield subsequent cost savings.
Additionally, the practice of EBM helps to eliminate fads, harmful practices, and outdated approaches. Physicians who practice EBM may improve their ability to discern between scientific and nonscientific information, gain increased awareness of bias, and develop an overall appreciation of the truth.
Finally, EBM promotes of a system of continuous training; the interconnection of medical assistance, education, and scientific research; pursuit of the best course of action while considering its effectiveness and potential risks; and selection of the most cost-effective or beneficial option for the patient.
CONCLUSION
The EBM revolution requires dedication, a critical outlook, and good medical practice. It mandates that physicians uphold primum non nocere and strive toward honest and respectful relationships with their patients. EBM prioritizes resource optimization, assessment of results by scientific methods and their publication, spreading of good science, and innovation. All of this should inspire and awaken enthusiasm, especially in the younger generation of ophthalmologists. EBM should be a source of guidance and motivation in our efforts to advance ophthalmology and to achieve the ambitious goals we set for our practice and patients.
1. Sackett DL. Evidence-Based Medicine. How to Practice and Teach EBM. 2nd ed. London: Churchill Livingstone; 2000.
2. Greenhalgh T. How to Read a Paper. The Basics of the Evidence-Based Medicine. 5th ed. Chichester, West Sussex: BMJ Books; 2014.
3. Junquera LM, Baladron J, Albertos JM, Olas S. Medicina basada en la evidencia: Ventajas. Rev Esp Cirug Oral y Maxilofac. 2003;25(5):265-272.



