A Maiden Surgical Voyage
The charm of the maiden voyage,
Could turn into a carnage;
For many a sailor in making,
Their dreams destroyed by hands shaking.
When those men assume they are on an even keel, joyfully heading for the docks;
Bamboozled by the perilous sea, they are veritably heading for the rocks.
Learning about the vessel from stem to stern,
To make headway courageously thwarting heartburn;
Then, some guidance from one knowing the ropes,
Is how the fledgling sailor copes.
The patient is ready for surgery. Are you?” quipped Pankaj Sharma, MBBS, MD, DNB. “I was born ready, Sir!” I riposted in jest. Beneath my calm façade, however, lay a heart quivering with fear, as I had just summarized the details of a prospective patient for my first solo surgery to my mentor, Professor Sharma.

Professor Sharma
A woman in a traditional Muslim veil had walked into the clinic one morning with hopes of gaining not just better vision, but a better life. A widow employed in semiprecious stonework near Jaipur, she needed to earn for her daughter’s future. A misconception in rural India is that women in the medical profession are nurses, so she was astounded to learn that I was, in fact, a doctor. She had a contemplative look when I informed her about her cataract and her surgical options. I saw a glint of hope in her eyes as she implored, “Would you guide my daughter to become a doctor like you? I want YOU to operate and show my daughter what girls can do!” I was yearning for my surgical debut, but this was something I could not have anticipated. By a strange quirk of fate, my incipient surgical career had been catapulted to a position of setting a precedent for women’s emancipation. Instead of replying immediately, I told her to proceed for her systemic examination, buying time to talk to my mentor.
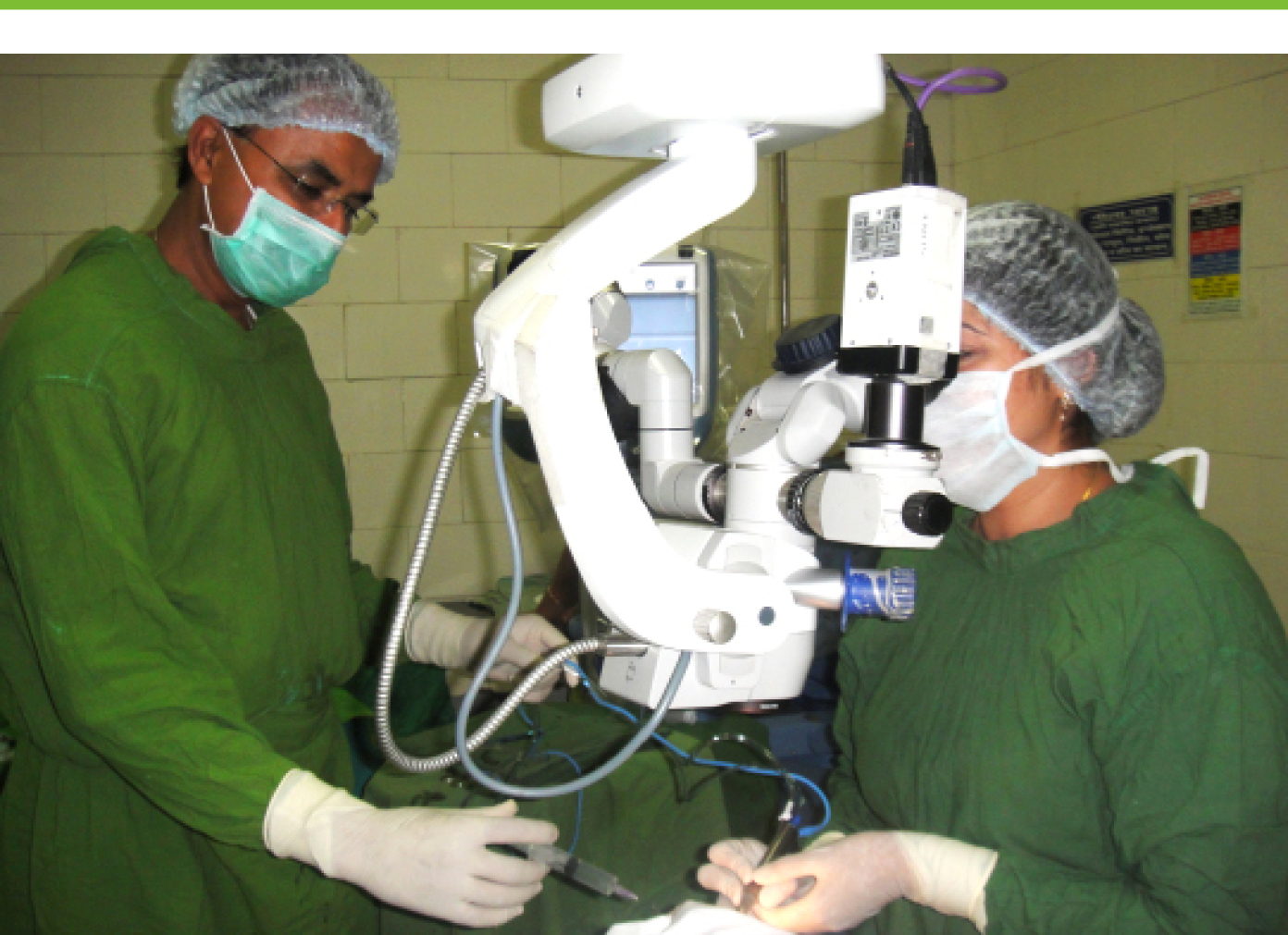
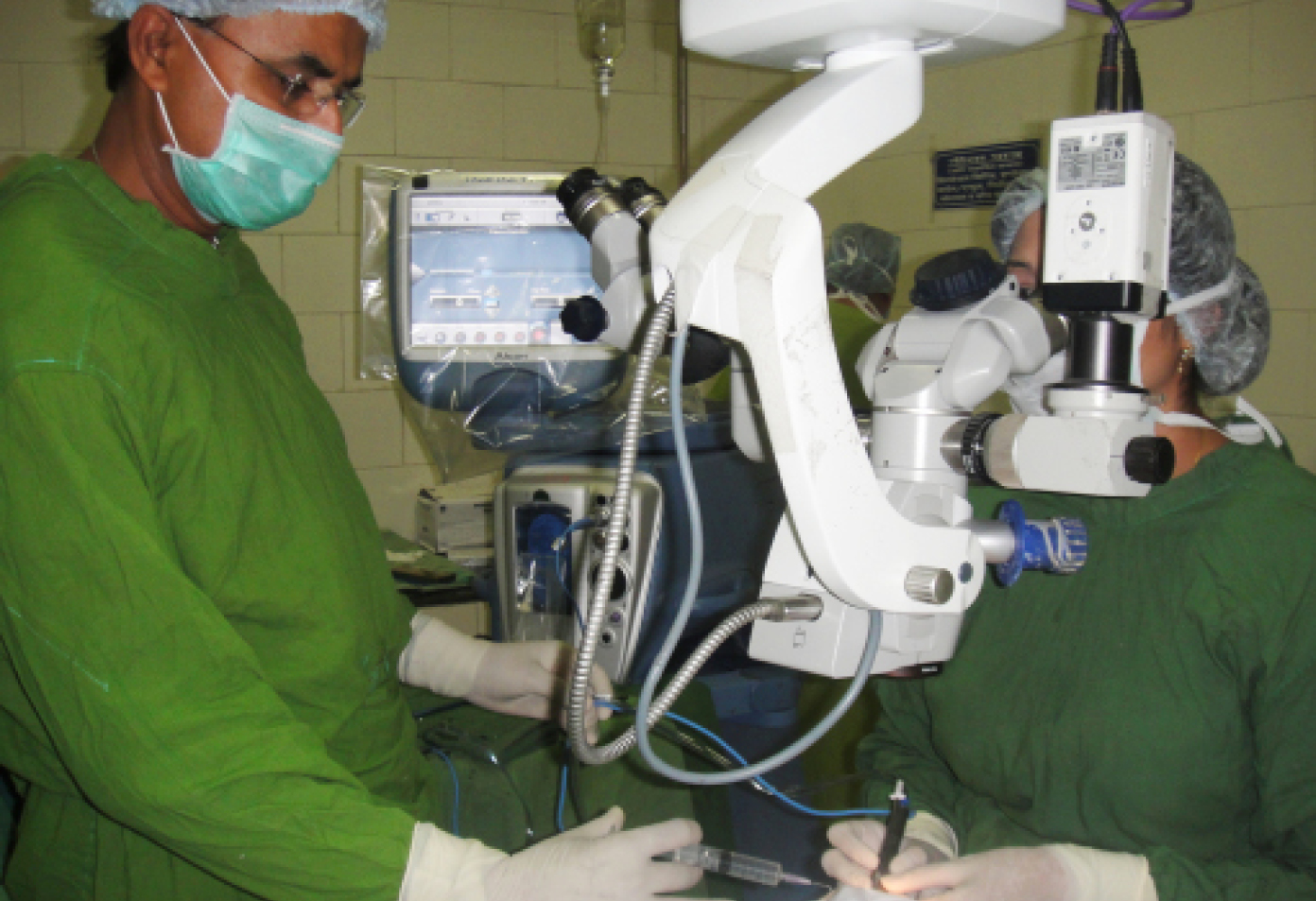
Dr. Kalia performing phacoemulsification under the guidance of Professor Sharma.
A detailed informed consent and my mentor’s erudite stance helped in my maiden surgical voyage. Books by Roger F. Steinert, MD, and Barry S. Seibel, MD, that I had devoured zealously became my beacon of light. Professor Sharma enunciated, “This grade 3 nucleus is apt, and you are reasonably proficient for your stage. Remember to respect the ocular tissues, especially the iris, endothelium, and posterior capsule, while maintaining the equipoise of pressure between the anterior and the posterior segments.”
The next day, I sought blessings from my parents before surgery. I had performed each step of phacoemulsification, albeit separately, in several cases under the guidance of a meticulous surgeon, and his faith in my abilities encouraged me. I felt that the way a play verged on montage, the OR, that day, had to be an amalgamation of all those steps. Praying to God to instill me with an imperturbable tranquillity for the impending surgical odyssey, I visualized my steps.

Dr. Kalia with her mentor Professor Sharma (second from left) at the 2013 ESCRS Meeting in Amsterdam.
Residents taunted me, “Even the Titanic made history!” I chose to reply with my actions. After scrubbing in, I draped the patient’s left eye, which was under peribulbar block, and looked at Professor Sharma for approval to begin. He positioned himself on the assistant scope and nodded, oblivious to my racing heartbeat. I fashioned a 1-mm sideport entry at 5 o’clock and filled the chamber with a cohesive ophthalmic viscosurgical device (OVD). Then, using a 2.8-mm keratome, I made a superotemporal three-step clear corneal incision at 2 o’clock. My fears were swept away with the wave of trypan blue that stained the anterior capsule (under OVD). I added a little more cohesive OVD before raising the capsulorhexis flap with Inamura forceps (Asico). It took me a while, and it was not the perfect circle I had envisioned, but slightly oval (about 4.5 mm x 5.5 mm). Because it was continuous, I could begin with phacoemulsification, after visualizing the fluid wave of hydrodissection and ensuring nuclear rotation.
After checking the three foot positions in the test chamber and adding dispersive OVD inside the eye, I ventured with my phaco probe. Instead of a chopper, I used a dialer (also known as a manipulator/modified Sinskey hook) and initially aspirated some superficial cortex. The Sovereign Compact Phacoemulsification System (Abbott Medical Optics) helped as I began the sculpting hesitantly with a few brief incursions at foot position 3. But Professor Sharma encouraged me to sculpt deeper without distorting the eye. As I pressed fully onto the foot pedal to deliver the maximum preset linear pulse power (60%) and sculpted a deep trench from the main incision to the opposite edge of the rhexis, I felt that the OR was percolating with an expectant energy. “Don’t push the nucleus; cut it with phaco” was the oft-repeated adage, which I remembered well. I rotated the nucleus to sculpt in a cross fashion. When the glow was partially visible, I tried to separate the two halves. The desired crack was produced when I went deeper in the trench. While I created four quadrants and refilled the anterior chamber with dispersive OVD, Professor Sharma changed the settings to flow rate: 36, maximum vacuum: 300, and power: 30% variable (WhiteStar Signature System [Abbott Medical Optics]). I mentally revised, “Hold, pull to the center, emulsify: 3, 2, 3” before tackling the first quadrant facing the main incision. Using the dialer and keeping the phaco tip in the center, one by one three pieces were eaten away.
Residents gathered near the surgical monitor. I was buoyed up by the phaco-assisted aspiration I had done, when a calm voice reminded me to be extremely careful while removing the last piece. I positioned the second instrument beneath the first, avoiding any jerky movements. I was relieved when this part was over, but I knew that the greatest chance of posterior capsular rent was in the next hurdle: irrigation/aspiration of the remaining cortex. So, with measured steps, I/A was completed. Next, I re-formed the capsular bag with a cohesive OVD before implanting a foldable IOL. The shores were in sight as I maneuvered the IOL into the bag. Maybe it was beginner’s luck, but I could finally relax after a quick aspiration of the OVD and wound hydration. My mentor’s announcement, “Sonal, celebrate!” was a pat on my back.
Postoperatively, the patient was happily employed again (BCVA: -6/9, N6), with a resolve to make her inspired daughter a doctor. I felt that although the journey is often more thrilling than the destination, sometimes a cruiser leads you to paradise!




