Evidence suggests that younger patients are at higher risk for corneal ectasia, which leaves them with poor vision and at an optical disadvantage. In the not-too-distant past, treatments for keratoconus, pellucid marginal degeneration, and postrefractive surgery ectasia were limited to contact lenses or corneal transplantation. Although corneal transplantation may be advantageous for many patients, it can lead to unacceptably high levels of astigmatism and poor visual outcomes in a significant minority. If the corneal transplant fails, we now know that subsequent transplants have a reduced chance of success.1 For a young person, this may mean many decades of poor vision.
With the advent of new technologies, the philosophy of cornea specialists has shifted from replacing ectatic corneal tissue by transplantation to strengthening and resculpting tissue to achieve better visual outcomes without the need for allografts and the inherent risks of that strategy.
Corneal collagen crosslinking (CXL) has been the foundation of this new approach. Without the ability to stabilize the cornea, it would not be possible to subsequently provide surgical refractive corrections yielding long-term visual rehabilitation.
Our preferred method at the Queen Victoria Hospital is to perform CXL in adults with progressive ectasia and in all children, unless contraindicated. We perform an epithelial disruption method that allows perfusion of the stroma with isotonic riboflavin, which takes a little longer than conventional epithelial debridement but carries the advantage of yielding less pain for less time, which is gratefully accepted by most patients. Results show that 84% of patients had a stable maximum keratometry (Kmax) at 12 months with this method. Despite the corneal stability as measured by tomography, BCVA remained stable in 55.4% of eyes and improved in 29.7%.2 The exact mechanism for this is debatable but may be related to the altered refractive index of the cornea after CXL.
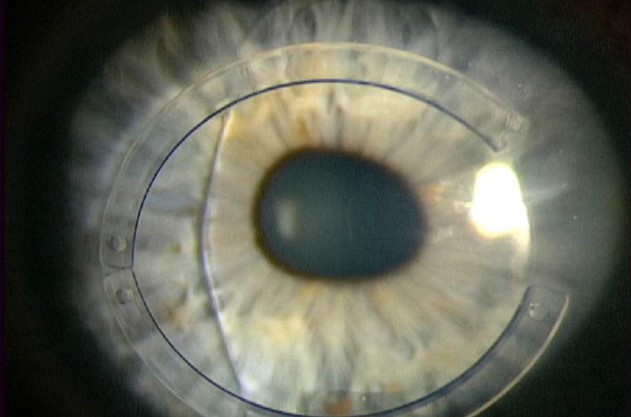
Following combination ICRS with CXL and phakic IOL implantation, this patient achieved 20/25 UCVA postoperatively.
Once corneal stability is achieved, the next step is surgical refractive improvement. If the patient’s corneal astigmatism is mainly regular and/or the phoropter allows refractive correction better than 20/40 (or the driving limit in the United Kingdom), the choice of treatment will depend on the status of the crystalline lens. Older patients (50 years plus) may benefit from either cataract surgery or clear lens extraction with implantation of a toric IOL.
The AT Torbi 709M (Carl Zeiss Meditec) allows up to 12.00 D of astigmatism correction. In our study, 75% of keratoconic patients implanted with the AT Torbi achieved a UCVA of 20/40 or better postoperatively. To achieve this, it must be appreciated that the ectatic cornea, like the normal cornea, produces a mixture of low- and higher-order aberrations. If the higher-order aberrations predominate, then correction of the low-order aberrations with a toric IOL will not produce an optimal outcome.3
For younger patients, if the anterior chamber morphology (depth, iridocorneal angle, crystalline lens curvature, endothelial cell count) is suitable and the astigmatism is regular and correctable with the phoropter, a toric phakic IOL can be offered. For patients with deep anterior chambers, the Artisan Toric lens (Ophtec) provides correction of up to 7.50 D of astigmatism and 23.50 D of myopic sphere. A sulcus-placed phakic lens (Visian ICL; STAAR Surgical) can correct up to 6.00 D of cylinder and 18.00 D of myopic sphere, but it lies in closer proximity to the crystalline lens in a patient group that is already more at risk of anterior subcapsular cataracts.
A more common scenario is to encounter a patient who, despite having undergone CXL, still has a high degree of irregular astigmatism that is not correctable by refraction. Treatment options in this case include topography-guided PRK for lower degrees of astigmatism and femtosecond laser intrastromal corneal ring segments for higher degrees. The goal of both of these approaches is not to produce improved UCVA, although that would be nice; instead, the aim is to improve BCVA with the intention of subsequently implanting a lens to perfect the spherocylindrical correction once stability of the preceding step is confirmed.
The advantage of this multistep treatment is that no allograft material is needed for these young patients, thus avoiding the need for lifelong graft management and all of the sight-threatening issues that entails. There are more primary procedures, but the outcome is better visual quality and less risk than with the now-historical open-sky penetrating keratoplasty.
1. Williams KA, Lowe MT, Keane MC, et al. The Australian Corneal Graft Registry 2012 Report. March 9, 2012. Available at https://dspace.flinders.edu.au/xmlui/handle/2328/25860. Accessed February 11, 2015.
2. Hirji N, Lam FC, Petraca R, Sykakis E, Hamada S, Lake D. Corneal collagen crosslinking for keratoconus without epithelial debridement. Eye. Accepted for publication.
3. Nanavaty M, Lake D, Daya S. Outcomes of pseudophakic toric intraocular lens implantation in keratoconic eyes. J Refract Surg. 2012;28(12):884-889.


